Audrey Labarre1,2, Gilles Tossing1,2, Claudia Maios1, James J Doyle1,3,4, and J Alex Parker1,2§
1Centre de Recherche du Centre Hospitalier de l'Université de Montréal (CRCHUM), Montreal, Canada.
2Department of Neuroscience, Université de Montréal, Montreal, Canada.
3Division of Experimental Medicine, Faculty of Medicine, McGill University, Montreal, Canada.
4Metabolic Disorders and Complications, Research Institute of the McGill University Health Centre , Montreal, Canada
§Correspondence to: J Alex Parker (ja.parker@umontreal.ca)
Abstract
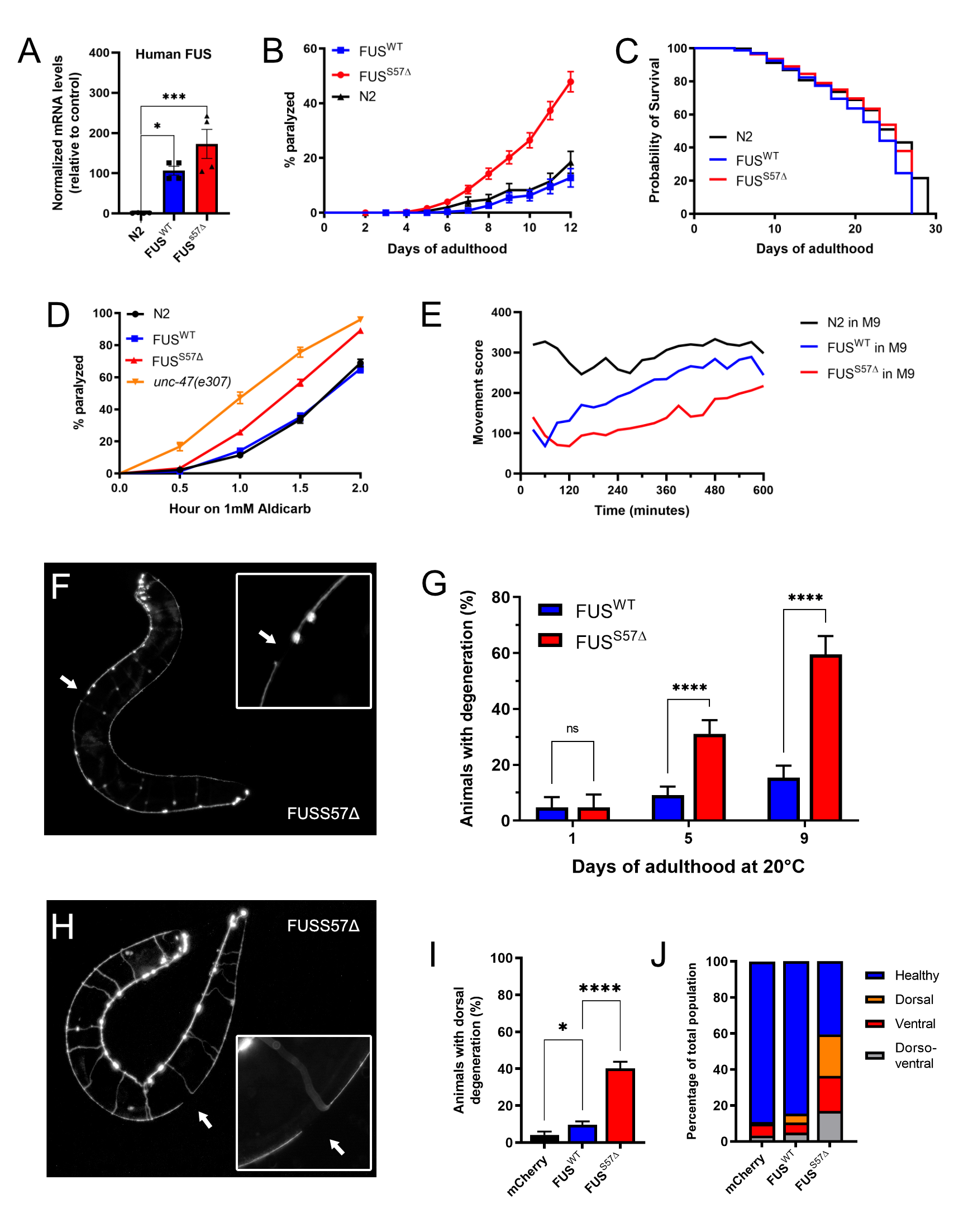
Description
Methods
Reagents
Acknowledgements
Funding
Author Contributions
- Audrey Labarre: Investigation, Formal analysis, Methodology, Validation, Writing - original draft
- Gilles Tossing: Investigation, Formal analysis, Methodology, Validation, Writing - original draft
- Claudia Maios: Investigation, Methodology, Validation
- James J Doyle: Writing - original draft
- J Alex Parker: Conceptualization, Funding acquisition, Supervision, Writing - review and editing
Reviewed By
Anonymous, Nicole Liachko
Nomenclature Validated By
Anonymous
Database Reference ID: WBPaper00061923
History
- Received: 8/3/2021
- Revision Received: 8/31/2021
- Accepted: 9/15/2021
- Published: 9/22/2021
Copyright
© 2021 by the authors. This is an open-access article distributed under the terms of the Creative Commons Attribution 4.0 International (CC BY 4.0) License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation
PubMed Central: PMC8459179
PubMed: 34568776

